Why Health Systems Matter: Ximena’s Story
Why Health Systems Matter: Ximena’s Story
We should never have met.
When I first met Ximena1 in 2016, she was breathing through a tube, relying on machines to keep her alive in the Intensive Care Unit at the prestigious teaching hospital where I worked in Boston. But she should not have been there; we never should have met. She was there, in so many ways, because the health system had failed her.
Ximena was originally from Guatemala and had come to the US several years earlier. Prior to migrating to South Carolina, she had successfully managed her diabetes for more than a decade and was doing well. She used insulin daily, maintaining her regimen without problems. Her doctors had told her that her diabetes was under control, and she had lost weight. Overall, she was thriving.
When she migrated to South Carolina, however, she did not have insurance. She quickly learned that in the US, insulin, needles, glucometers, test strips, and her other medications and supplies were prohibitively expensive without insurance. After trying to make ends meet for the first two months, she made the hard choice to go without her medications so she could buy food and pay rent for her family.
Two years passed. While Ximena was getting through her days just fine, she knew that her diabetes had gotten much worse. Using test strips borrowed from friends, she consistently saw that her blood sugar level was terribly high. She knew this would ultimately lead to problems, but she didn’t have the resources to do anything about it.
In 2016, she moved to Boston in response to an acquaintance’s promise of better work and came down with a cold a couple of weeks after arriving. Although such a minor illness had never been a problem for her before, she could tell this time was different.
Ximena became so ill that she was unable to work, and her boss sent her to the emergency room (ER) of the hospital where I worked. When she arrived, the wait was more than six hours long. Because there were no chairs to sit in, she stood in line as she became progressively weaker. A nurse Ximena turned to for help couldn’t understand Spanish and told her that an interpreter would be coming “in a few minutes.” That interpreter never appeared.
Sometime later, other patients waiting in line called for help after noticing Ximena lying unconscious on the floor. Blood was coming from her mouth, and she was completely unresponsive. The ER team rushed to the lobby and took over trying to revive her.
By the time I became involved several hours later, the team advised me that Ximena’s body was in a critical condition called diabetic ketoacidosis—a life-threatening complication of poorly managed diabetes. As my colleagues and I discussed her case, we hung our heads in shame: this was a completely preventable situation, and we all knew it.
At MSH, we work to strengthen health systems. But what does that actually mean?
There are many health systems frameworks out there, along with an extensive body of academic literature on the subject. But for simplicity’s sake, I like to think of a health system as a set of six “building blocks”2 that together make up an overall system that delivers the health services people need. Most importantly, the system is centered around the people themselves and designed according to their needs. I find this particular graphic3 to be helpful when trying to visualize how it all works:
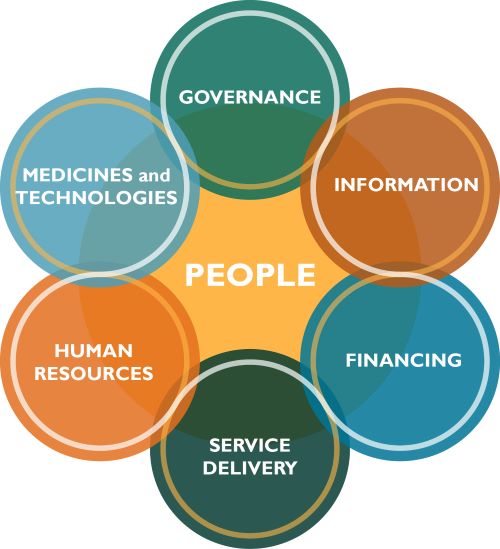
So, how does this framework help us understand Ximena’s story? When designed and managed well, each of these building blocks works in concert with the others to ensure that people receive high-quality, person-centered care when they need it. The reality, though, is that every health system in the world struggles to achieve these aspirational goals. As I reflect on Ximena’s story, I see clear gaps in all six of the building blocks—gaps that she ultimately fell through. Had our health system been stronger, her tragedy could have been prevented from ever happening.
- Governance: At the state level, South Carolina did not have policies in place that would have enabled Ximena to access health care without insurance.
- Financing: Because of her lack of health insurance, Ximena had to pay hundreds of dollars per month out-of-pocket for her insulin and other medications, which she could not afford.
- Medicines and technologies: Ximena’s lack of insulin and other medications caused her diabetes to progressively worsen, which led to her developing diabetic ketoacidosis and, ultimately, being hospitalized.
- Information: Although Ximena had longstanding relationships with her doctors in Guatemala, her medical records were never transmitted to the US and therefore were unavailable to help inform her care.
- Human resources: When Ximena arrived at the hospital in Boston, the ER was significantly understaffed with a long wait time, which resulted in her care being delayed. Furthermore, due to the language barrier, Ximena was unable to effectively communicate with the health workers.
- Service delivery: The ER’s lack of adequate staffing and hospital personnel’s inability to communicate with Ximena resulted in her life-threatening condition going unnoticed until she collapsed on the floor. Had the ER been able to provide more timely service, her condition could have been recognized and treated immediately and potentially resolved before it became critical.
Addressing the urgent need for person-centered health systems
Let me reiterate an important contextual detail: all of this happened in the US—which has the highest-cost health care system of any in the world—at one of the most prestigious teaching hospitals in the country. If such health systems failures can happen in this setting, it’s clear why other, more resource-constrained countries struggle to provide high-quality care to their communities.
The lesson is clear: to deliver on the human right to health and Sustainable Development Goal 3, we need strong, person-centered health systems. It is a sad reality that so many people around the world do not have access to high-quality health systems, and it further reinforces the foundational importance of the work we do at MSH every day.
Fortunately, Ximena’s story has a happy ending. After a few days in the hospital, she was able to return home to her family in good health. Moreover, due to the progressive policies in the state of Massachusetts—which themselves are a sign of good governance—we were able to enroll her in the state insurance program, connect her with a new primary care doctor, and get her back on her insulin and other medications. Seven years later, she is thriving and her diabetes is well-controlled.
Ximena always knew what she needed and wanted to make it happen—it was the system that prevented her from being healthy. Now, with a better health system, health abounds.
1 “Ximena” is a pseudonym used to protect the individual’s identity.
2 Monitoring the building blocks of health systems: a handbook and their management strategies; World Health Organization, 2010.