Combating Antimicrobial Resistance With Strong Coalitions: Implementation Experiences at the National and Regional Levels
Combating Antimicrobial Resistance With Strong Coalitions: Implementation Experiences at the National and Regional Levels
Read the journal article from Global Public Health
![[Participants of the EPN-SPS AMR regional workshop in Moshi, Tanzania. Photo credit: EPN]](https://msh.org/wp-content/uploads/2018/03/arm_817px.png)
Antimicrobial resistance (AMR) occurs when a microorganism becomes resistant to a drug that was originally effective for treating the infections it caused. It is one of the world’s most pressing global health threats and could erode progress made thus far in the treatment of HIV/AIDS, TB, malaria, and many other infectious diseases.
Management Sciences for Health’s (MSH) role in combatting AMR was recently featured in the peer-reviewed journal, Global Public Health.
The article describes an approach used by the USAID-funded Systems for Improved Access to Pharmaceuticals and Services (SIAPS) Program and its predecessors to build and strengthen coalitions to defeat AMR. SIAPS was implemented by MSH.
Because AMR is a complex issue that cannot be solved using a siloed approach, it requires coordination across sectors and stakeholders representing human and animal health, agriculture, and the environment. Forging coalitions can help achieve effective coordination and collaboration. Highlighting the importance of such coalitions, the 2015 WHO Global Action Plan on Antimicrobial Resistance calls for member states to “promote and support establishment of multisectoral (one-health) coalitions to address AMR at the local or national level, and participation in such coalitions at regional and global levels.” The emergence of coalitions could facilitate the development of national action plans, build consensus to advocate for policy change, raise awareness among professionals and the public, and provide leadership to implement antimicrobial stewardship and infection prevention and control interventions.
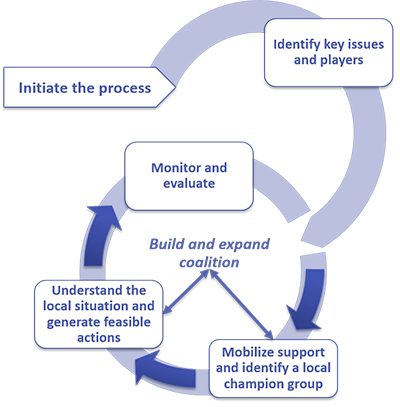
Based on its extensive country- and regional-level experiences, SIAPS has developed a practical guidebook on Building Coalitions for Containing Antimicrobial Resistance. This guidance document outlines the five-step coalition-building process: mobilize support, understand the local situation, develop an action plan, implement the plan, and monitor and evaluate. The document also provides step-by-step instructions, examples, tools, templates, and other resources.
Building effective coalitions require not only different actors from the public and private sectors but also strong leadership, a dedication to advocacy, and the need to consider the context in which it is being implemented.
In Zambia, for example, SIAPS identified stakeholders who were either interested or already engaged in AMR-related work. With initial support, the working group held a kick-off meeting and conducted a rapid assessment of the local situation. Using the results of the assessment, the group developed solutions that were specific to the context and a call-to-action document.
Besides Zambia, SIAPS and predecessors implemented the approach in Ethiopia and Namibia, and also at the regional level in collaboration with the Ecumenical Pharmaceutical Network (EPN), a faith-based regional organization. The newly published article describes the overall approach, implementation experiences, key results, challenges, and lessons learned that can inform the development of similar coalitions in other LMICs.
Since the complexity of AMR makes it too inefficient for one organization to comprehensively address it alone, coalitions can help bring various stakeholders together and amplify collaborations and actions. MSH’s Dr. Mohan P. Joshi and co-authors conclude in the article, “Our experience with the coalition-building approach … shows that coalitions can form in a variety of ways with many different stakeholders (i.e., government, academia, faith-based organizations) to generate a shared vision and carry out organized actions to preserve the effectiveness of existing antimicrobials and contain AMR.”
Article Citation: Mohan P. Joshi, Chifumbe Chintu, Mirfin Mpundu, Dan Kibuule, Oliver Hazemba, Tenaw Andualem, Martha Embrey, Bayobuya Phulu, and Heran Gerba. 2018. Multidisciplinary and multisectoral coalitions as catalysts for action against antimicrobial resistance: Implementation experiences at national and regional levels. Global Public Health. DOI: 10.1080/17441692.2018.1449230