Expert Voices: Dr. Alaine Nyaruhirira on Strong Laboratories Systems
Expert Voices: Dr. Alaine Nyaruhirira on Strong Laboratories Systems
Dr. Alaine Nyaruhirira is an expert in laboratories, diagnostics, and pharmaceutical and health systems strengthening. As a principal technical advisor at Management Sciences for Health (MSH), she provides global technical assistance to all lab-related projects across half a dozen countries, and she is part of a team working on interventions for laboratories and health systems strengthening to address global antimicrobial resistance and related climate change impacts on health systems. She led MSH’s panel session at the recent event with Mott MacDonald, and we asked her a few follow up questions about what’s next for strengthening lab systems.
The technical report you worked on with Mott MacDonald and ICF lays out challenges faced by lab systems in low- and middle-income countries, including weak governance and integration, vertical and unsustainable financing, maintaining a well-qualified workforce, and physical and operational infrastructure. Can you summarize what the biggest barriers are to addressing these?

Historically, labs have been a neglected piece in the health system. You’d go to a hospital and the lab would be a small room in the back or the basement. But with investment from programs like PEPFAR, more than 1,000 laboratories across Africa have now received accreditation, and we need to recognize the impact of programs like that.
At the same time, lack of leadership can be a bottleneck. In many countries, there isn’t a directorate sitting at the level of the Ministry of Health to elevate the voices of lab professionals and make a difference at the implementation level to encourage good conditions—labs with enough quality space and infrastructure to meet the demand from the community. Having a voice at the Ministry of Health level specifically for labs can help to formulate an implementable and costed strategic plan. This is the first gap I’m seeing and is one that could help us remove the other barriers.
The second gap is the availability of funds. If you look at the budget of a country’s Ministry of Health dedicated to hospital or health systems strengthening, how much is directed to labs and diagnostics?
Much of the funding to support diagnostics and lab strengthening comes from donors who make investments in specific health areas they’re trying to fight, like HIV, malaria, or tuberculosis (TB). I’d like to see more donors funding an integrated approach to lab work, which would include things like diabetes and other noncommunicable diseases. So, I think the two pillars we need to address are leadership (having good visibility of lab strengthening and diagnostic access) and funding.
To what extent was the scope of the COVID-19 pandemic attributable to a lack of strong lab systems? What difference could stronger lab systems have made?
Surveillance and communication among countries are crucial components of epidemic or pandemic preparedness and need a strong and functional lab system. COVID-19 is a good example of this.
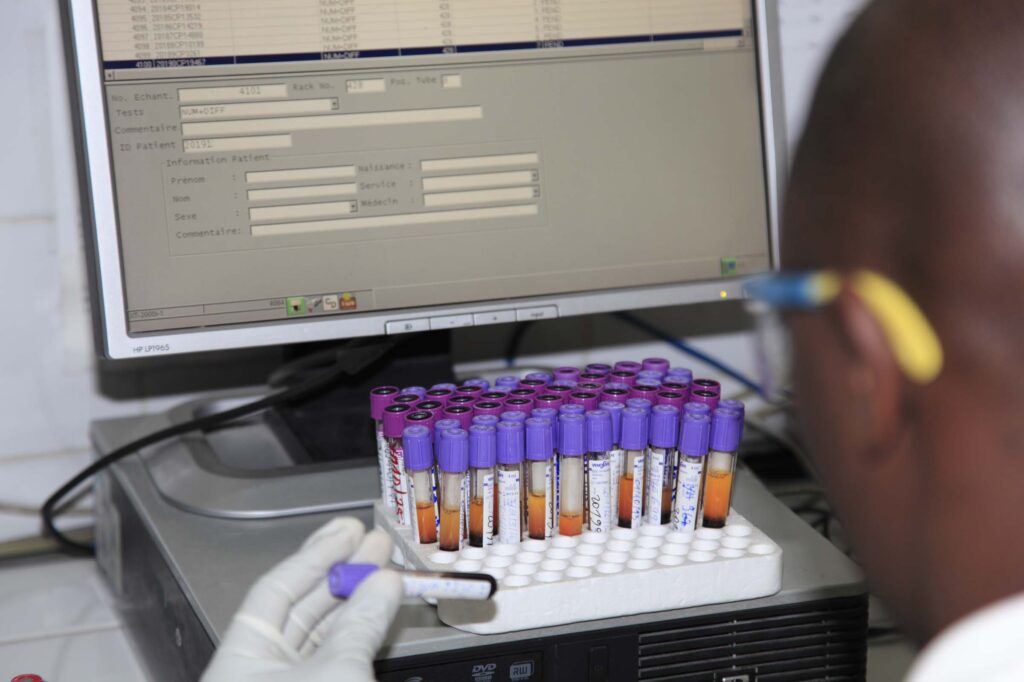
We must put surveillance systems, transparent data sharing, and accountability in place on a legal and policy level. In practice, a strong surveillance system means that you have human resources qualified to detect any threat quickly, and you have the tools and the platform to communicate across borders and globally.
For example, I traveled back to South Africa from Washington DC recently, and an outbreak of cholera had been declared in South Africa, Eswatini, and Mozambique. As soon as it was declared, the Africa Centres for Disease Control and Prevention (Africa CDC) sent out a communication and these countries began screening people at entry points. This is a case where everything worked well: at the leadership level, transparency at the country level, communication, and real-time surveillance at the community level. Surveillance can work only where detection can be made. Labs have a role in this by contributing human resources, equipment, and tests, among other things. When we talk about a system, it’s a combination of pillars that must be well coordinated in real time and supported by strong policy and leadership.
In its call to action, the Lancet Commission on Diagnostics report talked about the importance of involving lab professionals in decision making. What are we missing out on by not having their perspective?
We’ve started to be included more now! COVID taught everyone many lessons. For example, the African Society for Laboratory Medicine has launched the Laboratory Directors’ Forum, in partnership with Africa CDC, to form the basis for networking among African laboratory leaders.
It’s a start. But we need the resources, human resource capability, skilled technicians, and change of curricula at the academic level to be sure that lab technicians are finishing their academic programs well equipped. The perspective of laboratory professionals is critical. In addition, the landscape of technology is changing, and we are moving more and more from manual technology to automated machines, which means that lab technicians need to advocate for themselves and their colleagues to have the necessary computer skills.

Another challenge is that many tools and resources have been developed in English. But when you have to take a new lab machine to Angola, where they speak Portuguese, the user manuals need to be translated. We need to develop tools and protocols adapted to the right national and local languages. All of these things need to be done at the country level. Lab professionals know this and can be strong advocates for culturally relevant training materials.
There’s even more change on the horizon, with many tools being automated with artificial intelligence. The diagnostic landscape is evolving with rapid diagnostic testing, and some tasks could be shifted to community health workers. All of these things need a high level of skilled human resources, and lab professionals can help make sure facility-level needs are acknowledged in broader policies.
What do you think MSH’s unique contribution is around strengthening lab systems?

The first thing that sets MSH apart is that we were taking a systems thinking approach to our work before the term health systems strengthening became popular in the global health community. One way we do this around lab services integration is to adapt lessons learned in one country (like Ethiopia) and customizing them to another (like Afghanistan), looking at local epidemiology and demand for services. Even if the disease burden is vastly different (for example, Ethiopia has a much higher rate of HIV than Afghanistan), the patient needs for lab services are the same. In the case of GeneXpert technology, these machines can also test for hepatitis and COVID-19, which Afghanistan needs. We customize interventions across and within countries in a patient-centered way. Whether the patient is in Afghanistan, Ethiopia, or Rwanda, there will be different diseases and levels of demand.
The second strength of MSH is that we use local human resources. We strengthen the capacity of staff and the people we work with. It has been this way since MSH began. Wherever we are working, our mentorship approach means that when we close a project and come back with a new one, some of the same people will apply to work with us again. This means that they like MSH as an organization and that they come equipped with the skills and qualifications necessary for the project roles.
What gives you hope as you do this work?
I think there is good momentum around lab systems strengthening. COVID-19 taught is that there may be times when we cannot travel, seek service delivery next door, or even transfer samples from one facility to another or across country borders for testing. It’s important to build that capacity at the facility level. I think everyone at the global leadership level understands that. Some of that has been highlighted in this technical report.
For example, WHO has acknowledged the need for universal health coverage but has no clear position on diagnostics. At the World Health Assembly last May, the member states endorsed a resolution to strengthen diagnostics capacity and improve access to diagnostic services. And both the African and Southeast Asia Regional Offices of WHO have adopted their own continental roadmaps for health system resilience in emergencies that prioritize strengthening laboratory and diagnostic systems.
During COVID-19, the ACT accelerator mechanism was established, and one of the main pillars it acknowledged was diagnostics (along with therapeutics and vaccines). The Foundation for Innovative Diagnostic in Geneva is working with WHO to advance the research and development agenda around diagnostics to translate what we learn from research into real tools that can be deployed in the market. We now have a greater understanding at the continental level of the need for production of diagnostics and therapeutics in local markets, and regulations and institutions are being put in place. On the African continent, Africa CDC is leading some of these efforts. It’s good that all of this is now in place, but we still must translate global policy into country practice and have the right tools at the facility level. This linkage between global policy and the country level requires funding and donors—not only country-level domestic funding but also collaboration among donors. We have policy and advocacy tools available that we need to translate into implementable interventions to fight global diseases burden and prepare the world for emerging pandemic threats.
If you could tell people one thing about lab systems and know that they’d remember, what would that one thing be?
With a strong lab and surveillance system, we will be better prepared to face the next pandemic than we were when we faced COVID-19.