Transitioning a Health Care Workforce in Haiti’s Sud-Est Department
Transitioning a Health Care Workforce in Haiti’s Sud-Est Department
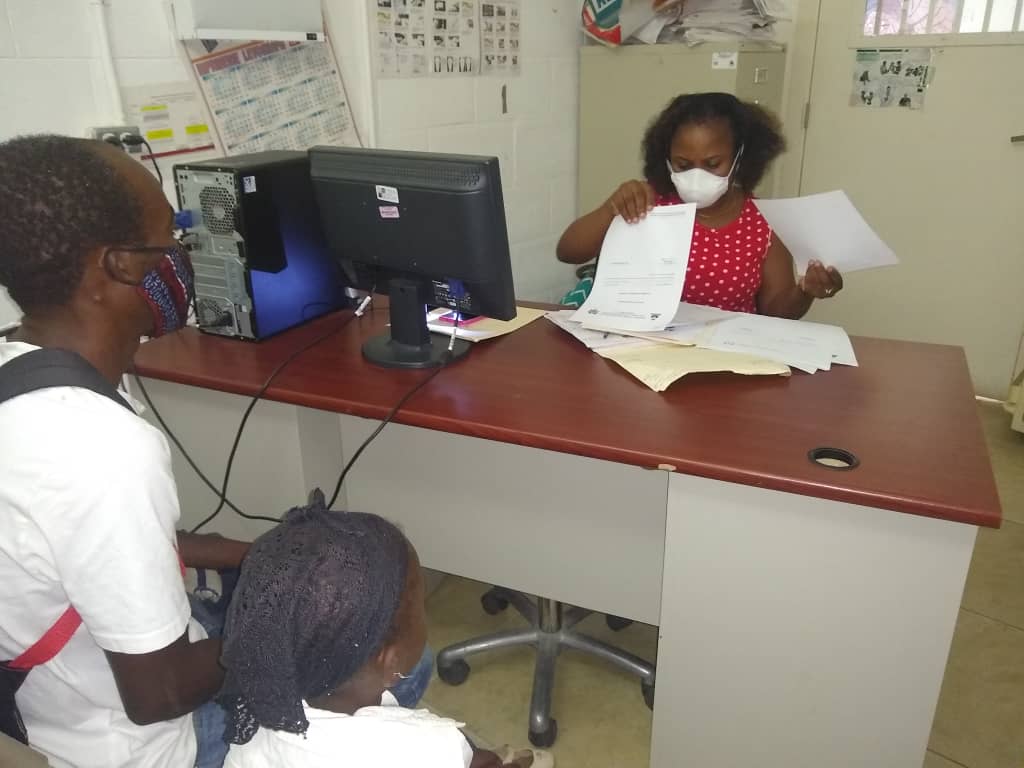
Health care workers are the backbone of a strong health system, and stabilizing the health workforce through reliable funding and efficient management strategies is crucial. But in Haiti, sustainable financing of human resources for health remains one of the biggest challenges facing the local health system, especially for the care of HIV patients.
Haiti has committed to UNAIDS’ 95-95-95 strategy: 95% of people living with HIV should know their HIV status; 95% of people who know their status should be on treatment; and 95% of people on treatment should have suppressed viral loads. However, the country is lagging behind on all indicators. The Ministère de la Santé Publique et de la Population (MSPP) reported that the most accurate data are 79-75-64 (Source: Monitoring and Evaluation and Integrated Surveillance/MESI-database, March 2021).
To reach these goals, it’s critical that health care facilities retain staff and prepare for economic challenges that could hinder future progress. Currently, 90% of staff in Haiti working in HIV/AIDS are paid full-time by the US President’s Emergency Plan for AIDS Relief (PEPFAR). If this donor funding were to suddenly end, efforts to achieve health-related Sustainable Development Goals, including UNAIDS’ 95-95-95 initiative, would be severely jeopardized. Most important, countless individuals living with HIV/AIDS in Haiti would lose access to the diagnosis and treatment services they desperately need.
A transition plan to sustain the health workforce
To get ahead of this issue before it’s too late, the MSPP, in collaboration with the USAID Health Leadership Project (HLP), began working to gradually absorb HIV health workers previously paid by PEPFAR into the government’s budget. A transition plan was developed by the MSPP and HLP to support the process of having the Haitian government directly pay the salaries of nearly 5,000 donor-paid HIV health care providers and community outreach workers by 2030 (Source: Transition Plan, Sept. 2020).
To help protect the well-being of staff and ensure a smooth transition across all facilities, HLP worked with the Direction des Ressources Humaines of the MSPP to develop guidance for how health departments should start this process. The first recommendation suggests transitioning all PEPFAR-funded staff in a health facility at the same time. This ensures uniformity across the department. Second, instead of automatically transferring staff, HR departments should follow their normal recruitment process and publish openings with specific job descriptions. This way, facilities can be confident that new hires have the skills they need to successfully do their jobs and that health staff knows exactly what is expected of them upon being hired. Lastly, it is recommended that facilities not hire people into HIV care-specific jobs but instead rotate all qualified staff through assignments. HIV care work can be physically and emotionally taxing, and rotating staff helps promote greater equity in job duties and allows departments to evenly share the load.
A cautionary tale
The initial rollout of the transition plan faced challenges in health departments that failed to follow these recommendations. For example, in the Nord and Nord-Est departments, facilities did not rotate all staff through services but instead recruited the PEPFAR-funded HIV care staff to only fill HIV care positions. This became a problem because the health personnel currently paid by PEPFAR are short-term contractors and are paid slightly higher salaries than their counterparts who are longer-term government employees. When these former contract workers accept government jobs, they are paid within the same salary scale as their colleagues. This left many HIV care staff unhappy, as they resented being asked to do the same job for a lower salary. As a result, five of the nine staff who transitioned in the Nord and Nord-Est departments refused to work on HIV activities without additional incentives.
Retaining health care workers throughout this transitional phase is crucial. The issues that occurred in the Nord and Nord-Est departments could have been avoided if these facilities followed the guidance and fairly distributed job duties among staff.

A model for success
Despite the issues that have come up in some facilities, this plan can be carried out successfully when the proper steps are taken to effectively manage staff. The Sud-Est department provides a strong example of how following the operational guidance can lead to a seamless transition of staff. The Département Sanitaire du Sud-Est (DSSE) successfully transitioned 10 health professionals from the Hôpital Saint-Michel de Jacmel (urban), the health center of Cayes Jacmel (medium sized), and the health center of Thiotte (rural).
Unlike the Nord and Nord-Est departments, the DSSE rotated its staff through all services. Additionally, the DSSE recognized that staff take on a greater workload when providing HIV care and offered financial incentives to all staff when they are on this service. The funding for these additional incentives is currently coming from PEPFAR, but the DSSE hopes that the positive work they are doing will encourage the MSPP to extend its results-based financing program to its facilities to cover the costs. This program rewards facilities and staff that meet set performance targets. Offering these incentives not only helps retain staff but also sends the message that their hard work is acknowledged and appreciated.
As the rollout of the transition plan ramps up, the Sud-Est department is a good model for other departments to follow. The fact that this approach was successful across a range of facilities, including an urban hospital, medium-sized health center, and rural health center, shows that this plan can work universally. HLP will be sharing these lessons widely so that more facilities can implement this plan. While helping to solve one problem, this transition also represents an important step forward in creating a stabilized financial management system that is not dependent on unreliable donor funding. In turn, these health systems can more easily recruit and retain staff and focus on providing Haitians with lifesaving medical care.
“The absorption of staff that was previously paid by donors’ agencies, specifically for HIV, shouldn’t be considered as an isolated intervention but as an integral part of the plan to strengthen the workforce for the care of the population.”
Ms. Zita Dominique Paul, nursing care coordinator for the Hôpital Saint-Michel de Jacmel and one of the health staff transferred