PHC Leadership Development Program Facilitation Guides
PHC Leadership Development Program (PHC-LDP) Facilitation Guides

About this resource
The PHC Leadership Development Program (PHC-LDP) facilitation guides provide practical, step-by-step guidance for strengthening how district health teams lead, manage, and improve primary health care (PHC) systems.
Adapted from Management Sciences for Health’s Leadership Development Program (LDP) and Leadership Development Program Plus (LDP+), first introduced in 2002 and applied in more than 80 countries — these guides translate a proven, results-oriented methodology into the context of district-led PHC systems. They are designed for facilitators working alongside District Health Management Teams (DHMTs) and other subnational leaders to address real service delivery challenges using their own data, within their own systems.
Rather than focusing on individual leadership traits, the PHC-LDP emphasizes leading, managing, and governing as observable practices that teams can learn, apply, and strengthen over time. DHMTs work on real challenges using their own data, receive coaching and peer support, and progress through structured improvement cycles embedded in their routine management processes.
The PHC-LDP is implemented as a core component of the PHC-PM Activity operating alongside integrated district PHC dashboards, MEL systems, and catalytic grant support — together enabling DHMTs to continuously analyze, act, learn, and adapt as stewards of their district health system.
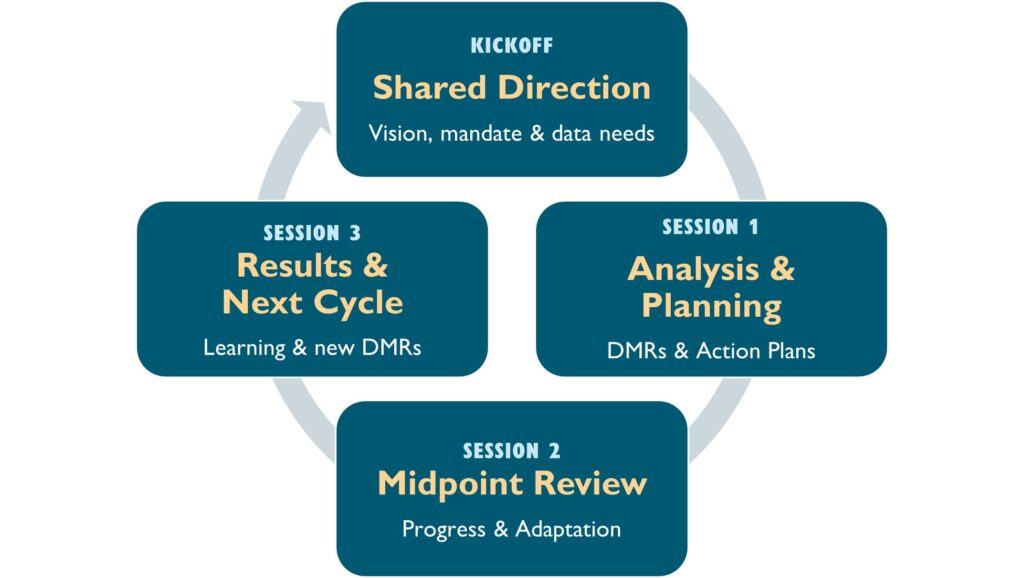
The PHC-LDP improvement cycle:
Each six-month PHC-LDP cycle aligns with the rhythm of DHMT quarterly meetings and is designed to repeat — with teams addressing desired measurable results (DMRs) and each cycle building on the last.
What’s included in this resource
The PHC-LDP resource collection includes facilitation guides, action planning tools, coaching resources, and M&E materials — all designed to be adapted to local context while preserving core methodology.

Facilitation guides
- Introduction & User Guide
- Kickoff: Setting Shared Direction
- Session 1: Identifying PHC Challenges
- Session 2: Midpoint Review
- Session 3: Results & What’s Next
Action planning tools
- Action Plan Template
- Challenge Model Worksheet
- PHC Improvements Roadmap/Calendar
- Actor Mapping Template


M&E resources
- M&E Planning Worksheet
- DMR tracking spreadsheets
Coaching resources
- PHC-LDP Coaching Guide & Resources
- Leading, Managing, & Governing practices handout and conceptual model

Request the guides

Complete the request form to receive the full guide series and supporting materials, or contact MSH Communications team directly at [email protected].
Related stories & applications
Coming soon. Check back for updates.