Behind the Supply Chain Scene: Keeping Nigerian Children Safe from Malaria
Behind the Supply Chain Scene: Keeping Nigerian Children Safe from Malaria
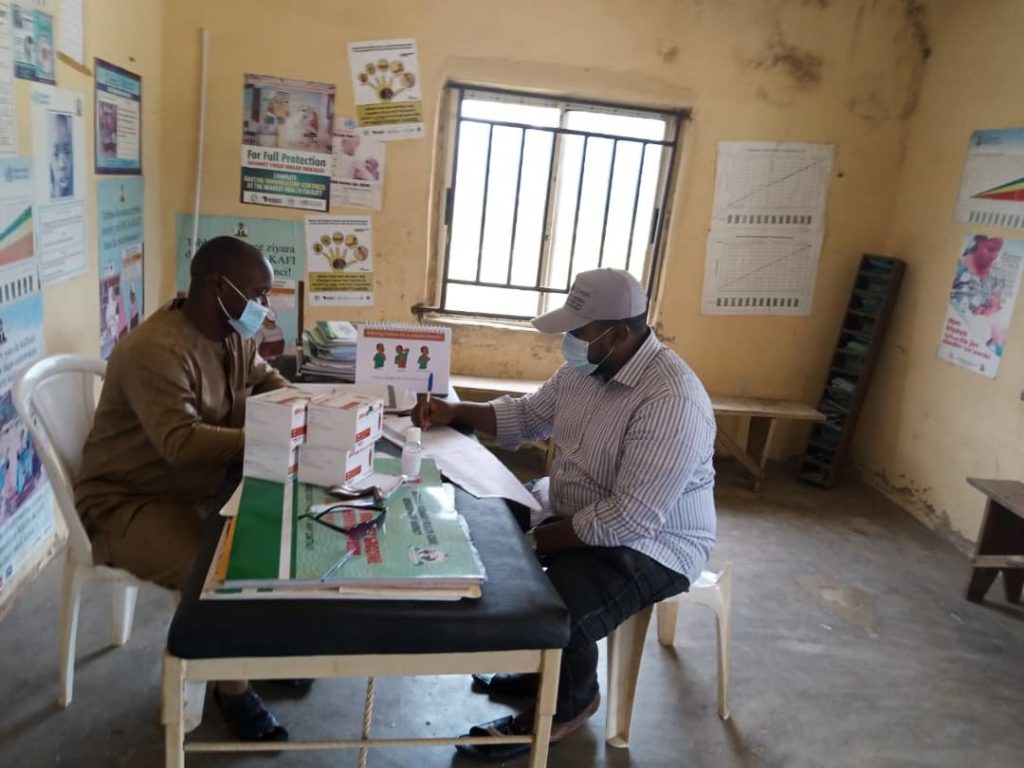
Last year, during the rainy season—when malaria risk increases—Management Sciences for Health’s supply chain team ensured continuous availability of medicines to prevent malaria through campaigns to reach children in the states of Taraba and Katsina.
What does it take for a lifesaving malaria drug to move from the manufacturing plant to the patient who needs it in hard-to-reach communities?
Under ideal circumstances, ensuring availability and accessibility of medicines takes coordination and expertise—a challenge even greater in countries with weak or inconsistent infrastructure. The complexity increases in rural or isolated communities.
In Nigeria—home to roughly a quarter of the world’s malaria cases and almost 32% of all malaria deaths—MSH, in partnership with Catholic Relief Services (CRS) and the National Malaria Elimination Program (NMEP), with funding from the Global Fund, set out to reach children under five with medicines to prevent malaria during the rainy season. The intervention involves administering monthly doses of antimalarial drugs to prevent malaria in those most vulnerable to the disease’s effects (in this case, children aged 3-59 months) during peak malaria transmission season. This is known as seasonal malaria chemoprevention campaigns.
The work took place in Taraba and Katsina States, where most of the population lives in rural areas with suboptimal health systems.
Here’s a look behind the scenes at how MSH helped shore up links in the supply chain to make the effort a success.
Training front-line personnel
In partnership with CRS and NMEP, MSH helped develop guidance for health facility workers on proper inventory management of antimalarials and appropriate use of personal protective equipment (PPE).
Using the national strategy and guidance for implementing seasonal malaria chemoprevention, MSH employed a train-the-trainer approach to train campaign consultants and state government teams, who, in turn, trained health facility personnel and community volunteers—town announcers, lead mothers (experienced caregivers), and community drug distributors—on proper filling of records, handling, and daily reconciliation of antimalarials.
MSH supported the states in training 3,444 health workers in Katsina and 708 health workers in Taraba. MSH also trained 15,651 drug dispensers, 2,429 lead mothers, and 2,432 town announcers in both states. These community members should be available to support subsequent cycles of the campaign.
Assessing and upgrading medicine warehouses
In coordination with state ministries of health, CRS, and NMEP, MSH assessed the adequacy of the warehouses, the first stop the medicine makes in the state from the manufacturer: Were the stockrooms the right size and structurally sound? Were their roofs intact and able to withstand copious amounts of rainfall? Could they maintain the proper temperature to preserve the medicines? Did they have safety, security, housekeeping, and inventory management protocols in place? These were some of the key assessment questions.
Once the state governments made the upgrades identified in our assessments, the Central Medical Stores in Katsina and Taraba were deemed ideal locations to store the medicines for the campaigns.
Managing inventories and transportation
When the medicines arrived at the Central Medical Stores, MSH coordinated receipt and storage. Each shipment was inspected, counted, and the accompanying waybills completed before the medicines were inventoried and properly stored prior to the next leg of the journey.
The governments of both states provided vehicles to transport the medicines to 2,060 health facilities, which were chosen based on the number of eligible children that each would serve during each campaign cycle. The distribution plans accounted for the quantity of antimalarials needed in each location and all necessary PPE to prevent COVID-19. In each cycle, more than 40 containerized vehicles were deployed to transport these health products. Sometimes it took more than 24 hours to reach some health facilities, especially in difficult terrains that are worsened by rainfall. The states coordinated this transportation with oversight support and monitoring from MSH and CRS. Deliveries were, in most cases, completed at least one day before the campaign launched.
The medicines were counted upon arrival at each facility to ensure they tallied with the quantities in the waybills before they were received. Such measures exist to prevent medicines from being stolen for sale in the open market. To avoid stock-outs—while guaranteeing these commodities were appropriately accounted for during the campaigns—state government personnel and MSH staff compiled daily reports showing the number of doses administered to eligible children and the quantities available at each facility.
Launching distribution of antimalarials
The campaigns are carried out by teams comprised of two community drug distributors and one town announcer, whose role is to create awareness of the intervention at the community level by using a megaphone.
Each team is expected to cover 70 children per day for 4 days during each campaign cycle. A health facility worker supervises four teams, making sure the administration of antimalarials is done correctly.
Community drug distributors typically play the unique role of dispensing the first dose on day 1 of these drug distribution campaigns, and then providing the children’s caregivers with guidance for administering the medicines on days 2 and 3. But given the COVID-19 pandemic, their role was modified to that of observer, guiding the caregivers to administer the first dose.
Following the administration of the first dose, lead mothers visited each household to confirm caregivers have given the second and third doses. Where caregivers had yet to give the medicine, lead mothers ensured they did so before moving to another household.
Reallocating surplus medicines and assessing results
Finally, MSH supported reverse logistics for unused medicines. First, local government logistics officers verify unused medicines returned by the health facilities and document their quantities before transporting them back to the Central Medical Stores. Second, returned quantities are verified at the stores, entered in the stock cards, and incorporated into the stocks of those warehouses. The stock balance at the end of each cycle is verified.
One key outcome of the campaign is in the strengthened health system that MSH and our partners helped forge working with state governments, especially regarding supply chain management.
The campaigns exceeded our goals: 2.1 million children were treated in Katsina, relative to the target of 1,886,259; 433,000 were treated in Taraba, relative to the target of 400,238.
With a strengthened health workforce and an improved supply chain for antimalarials, Taraba and Katsina States are poised to continue yearly campaigns. At MSH, we’re ready to support the rest of Nigeria and other countries where the scourge of this age-old disease is still a threat.