In a Pandemic, Put the Last Mile First
In a Pandemic, Put the Last Mile First
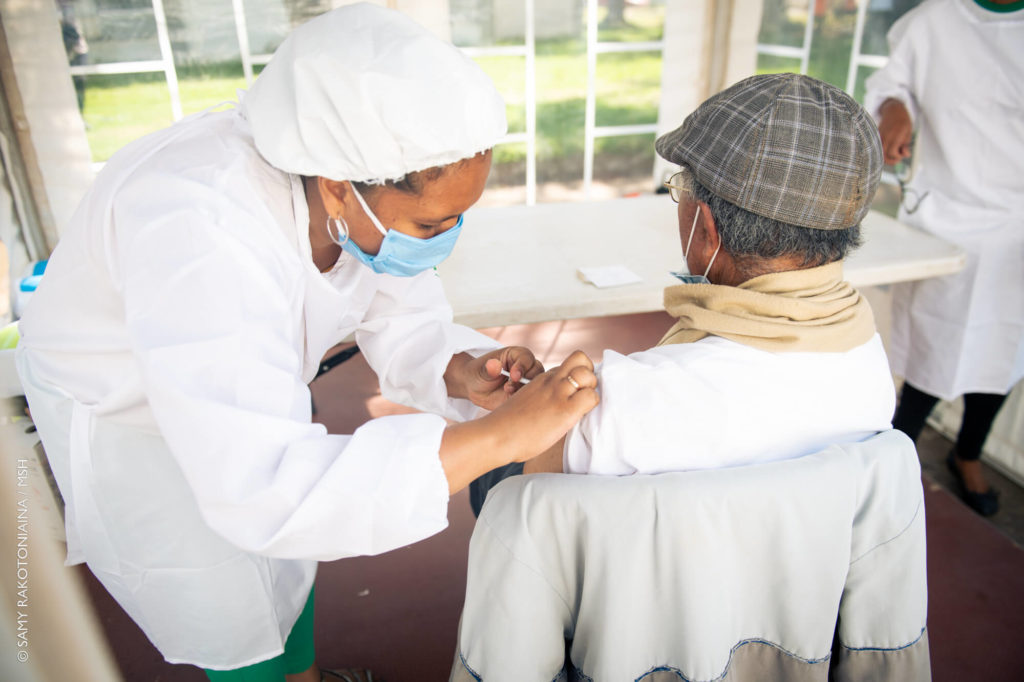
The past 10 days have seen a flurry of new US initiatives to meet the World Health Organizations target of vaccinating 70% of the global population – including a new Global Action Plan; involvement of PEPFAR networks to strengthen health system response; and most recently, a special US thrust in Nigeria, the continent’s most populous nation.
Underlining these efforts, as noted by US Secretary of State Antony Blinken in his announcement of the GAP plan, is the urgency of solving so-called ‘last mile’ challenges, like access to cold storage for transporting vaccines to places of implementation. Along with generating demand for vaccines, strengthening community health systems is a vital part of bringing the pandemic to an end.
At the same time, we are seeing developed countries finally moving on from the pandemic. Europe is lifting COVID restrictions. Most US states are abandoning mask mandates, and even countries such as Australia are finally reopening to tourists – steps Africa took some months ago.
Prioritizing the last mile – investing in the future
But there is a danger, as societies move on – leaving global health agencies to carry out the unfinished business of vaccinating the world – that we will quickly forget the lessons of the last two years.
If we only focus on the moment, we will not invest in what needs to be done for the future, to meet the next outbreak, when it happens.
In addition, it is essential that we do not forget the importance of investing in local capacity, primary health care and disaster management.
The next disease outbreak, just like this one, will begin at the household and community level and reverberate outward as infections spread – we need, therefore, to put the “last mile” first and prioritize local solutions. Vaccines take time to develop and even longer to roll out. Local jurisdictions must be able to respond without waiting for assistance from often overtaxed national health care systems. As we’ve seen throughout the pandemic, a country’s success or failure will correlate with the aggregation of local efforts.
From the lessons of the last two years, we recommend action on three fronts:
1. Act local
National preparedness and response plans, including mitigation policies and vaccination and testing campaigns, must include training of local responders on the ground. These plans should include a pandemic planning scenario and be informed by a multisector, whole government approach with local flexibility.
Local jurisdictions also need a legal framework established by the central government that gives them authority for early action. Without this, time is lost, and the window for containment closes. If they have the authority to act, and act quickly, local leaders are better able to manage the response, provide public messaging and risk communication, engage communities, and make key policy decisions.
2. Don’t forget about the importance of primary care and resilience of the public health infrastructure
Who can forget the images of overwhelmed hospitals from New York to South Africa, with makeshift morgues and patients on gurneys clogging crowded hospital halls? Years into the pandemic, we’re now learning of collateral damage: significant excess deaths as cancer, TB, and other diseases go undiagnosed and untreated by overwhelmed hospitals or because people avoid health care institutions. These examples reflect the challenges in pivoting to triage care in a health emergency.
Two capabilities are therefore needed when health system resources are overwhelmed: a framework to identify nonessential services that can be temporarily halted and the resources diverted to essential care, including non-pandemic essential care, and a holistic approach to identify additional capacity in the community so resources can be triaged to save the most lives.
3. Give public health a seat at the table with disaster management agencies
Pandemic preparedness and response must be fully integrated into existing disaster management agencies at the national and subnational levels. Multisector plans that provide for incident management and cross-sectoral collaboration and include continuity of essential operations should be developed and routinely exercised at the national and local levels.
For example, the ability to transport medical supplies or set up security at mass vaccination sites cannot be handled by public health officials alone. The funding mechanisms, surge personnel, and expertise from the other sectors need to be accessed and coordinated through a single management entity.
What’s needed are routine, annual exercises that reflect actual national and local plans and include the people who will be tasked with responding. Simulations geared to the highest levels are important, but insufficient.
The nonprofit global health organization we work for, Management Sciences for Health, offers a toolkit for local leaders, in low resource settings to help with these efforts.
Let’s build on the protocols and strategies developed throughout this pandemic and not forget the lessons learned as the current crisis eases. There will be another one, and we must be better prepared than we are now.
Elke Konings, PhD, MSc, is a senior director for pandemic preparedness, response and recovery at Management Sciences for Health, a nonprofit global health organization.
Lisa Stone, MD, MPH, is a pandemic preparedness and response consultant.
Press Contact
Please direct all press inquiries to Jordan Coriza at [email protected] or 617-250-9107