Resources
Resources
In partnership with countries around the world, we have developed hundreds of resources to help strengthen the foundations of health systems. Please search our Resources to learn more about our publications, research, programmatic approaches, tools, and learnings.

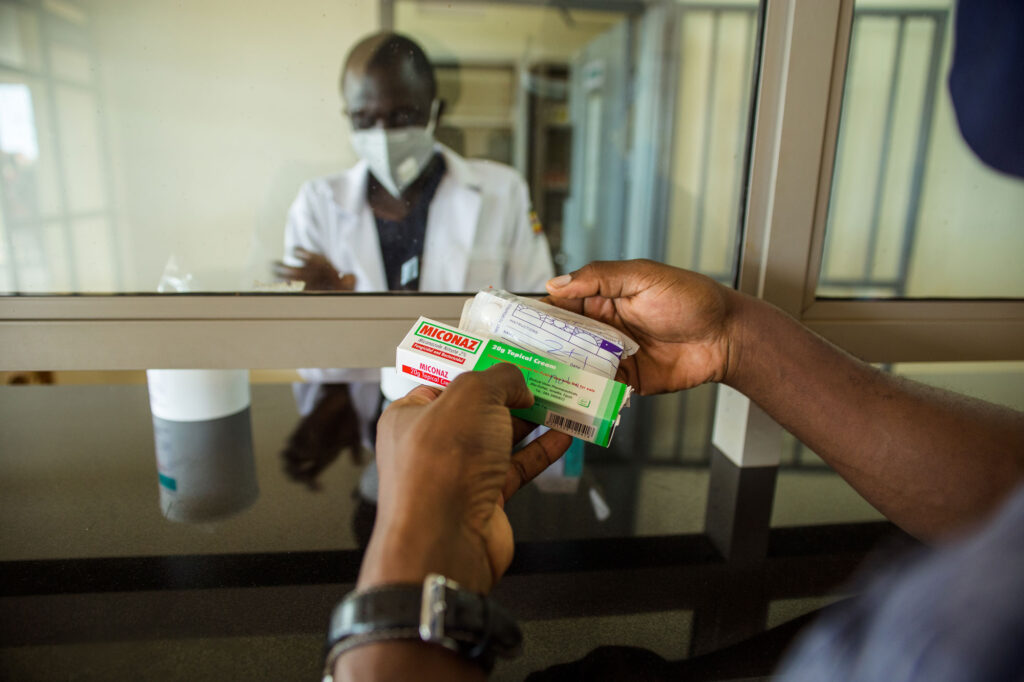
Strengthening Supply Chain and Pharmaceutical Systems for Sustained Health Impact
For more than three decades, Management Sciences for Health (MSH) has partnered with countries to build high-performing supply chains that ensure reliable access to safe, effective, quality-assured medicines and people-centered pharmaceutical services. MSH takes a holistic approach that fosters country-led innovation, whole-of-society engagement and collaboration, private-sector engagement, and effective leadership and governance. This ensures both reliable, affordable access to and sustainable delivery of medical products when and where they are needed and their appropriate use to save lives and improve health.
Topical
Estimating the opportunity cost of seasonal malaria chemoprevention implementation in Burkina Faso, Mali and Senegal
This study assesses the economic viability of expanding malaria community case management to all ages in Farafangana district, Madagascar.
Safe, Affordable, and Effective Medicines for Ukrainians (SAFEMed) Activity – September 2025 Monthly Newsletter
Transforming Digital Health in Ukraine
Estimating the opportunity cost of seasonal malaria chemoprevention implementation in Burkina Faso, Mali and Senegal
This study assesses the economic viability of expanding malaria community case management to all ages in Farafangana district, Madagascar.

Safe, Affordable, and Effective Medicines for Ukrainians (SAFEMed) Activity – September 2025 Monthly Newsletter

Establishment and Operationalization of the State Control Authority in Ukraine

Annual Report 2024: Strong Health Systems Save Lives

Antimicrobial Resistance (AMR) Alert – Edition 2: Strengthening Frontlines Capacity and Data-Driven Action for AMR Surveillance in Nigeria

Tackling Antimicrobial Resistance (AMR) in Nigeria’s Animal Health Sector: Policy Actions for a Sustainable Future

Strengthening Antimicrobial Resistance (AMR) Surveillance in Nigeria: An Urgent Call for Coordinated Action

Antimicrobial Resistance (AMR) Alert – Edition 1: Kickstarting Phase II of AMR Surveillance in Nigeria

Safe, Affordable, and Effective Medicines for Ukrainians (SAFEMed) Activity – August 2025 Monthly Newsletter

Strengthening Foundations, Driving Impact: A Model for District-led PHC Transformation

